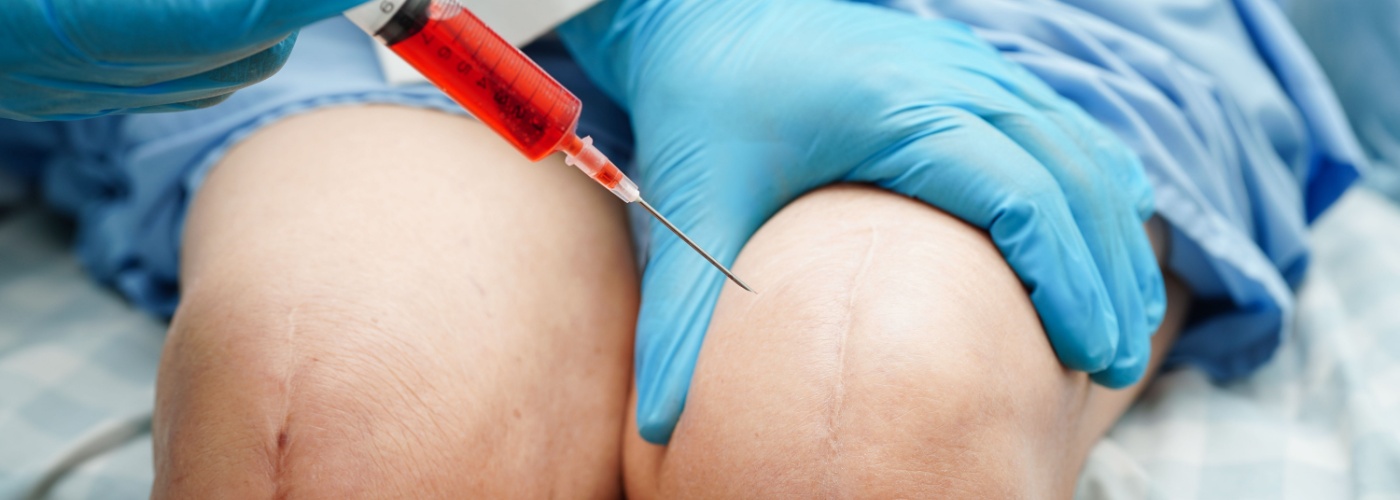
Many people live with joint pain, tendon injuries, or arthritis. Two common options are regenerative care or an operation. This guide explains stem cell therapy vs surgery in simple terms.
Differences in Regenerative Stem Cell Therapy vs Surgery
Stem Cell Therapy vs Surgery compares two different ways to address damage. Stem cell therapy aims to support healing inside the tissue. It often uses your own cells to signal repair.
Surgery changes the body structure more directly. It may remove torn tissue or replace worn surfaces. Both approaches can reduce pain and improve movement.
Stem cell therapy is usually minimally invasive and clinic-based. Many treatments involve a needle and imaging guidance. Surgery usually needs an operating room and anesthesia.
Recovery often includes wound care and activity limits. Stem cell therapy tries to restore function with less tissue disruption. Surgery may be needed when the damage is too advanced.
The best option depends on the diagnosis and your goals. Some problems respond to rehab and injections. Others require a repair that only surgery can provide. Imaging findings help guide the decision.
Symptoms and daily limits also matter. A good plan matches the condition stage, not just the pain level.
What Happens During a Stem Cell Injection Procedure?
A stem cell procedure often starts with a cell collection step. Doctors may collect bone marrow from the pelvis. Some clinics use fat tissue as another source. The sample is processed to concentrate helpful cells. This step may also concentrate growth factors. The final product is prepared for injection into the target area.
The injection is placed using ultrasound or X-ray guidance. This helps accuracy and protects nearby structures. The visit is often outpatient and shorter than surgery. You may rest briefly, then go home.
Most patients choose this route to avoid incisions and hospital admission. You may be given activity limits for a short period.
Healing usually happens over weeks, not overnight. Some soreness can occur after the injection. Swelling can also happen for a few days. Doctors may recommend physical therapy or gradual loading.
Progress is tracked with function, not just pain. Results vary based on the tissue and the injury stage.
Risks & Benefits of Surgery
Surgery can be very helpful for severe structural problems. Examples include unstable joints or major tears. Surgeons can repair tissue, remove fragments, or replace joints. This can restore alignment and improve stability.
Some procedures provide rapid mechanical improvement. Many patients regain activity after rehab and strengthening.
Surgery also brings real risks that must be considered. Infection can occur, even with careful sterile technique. Blood clots are a concern after some operations. Nerve irritation or stiffness can also happen.
Recovery can take weeks or months, depending on the procedure. Surgery can work well, but it demands downtime and carries a higher complication risk.
Some surgeries may need future procedures later in life. Artificial joints can wear and loosen over time. Scar tissue can limit range of motion for some patients. Rehab is often required for the best outcome.
Your overall health can affect surgical recovery. A surgeon should explain your personal risk profile clearly.
Comparing Long-Term Outcomes and Success Rates
Long-term outcomes depend on the condition being treated. Stem cell therapy may reduce inflammation and improve function. It may help certain tendon or cartilage problems.
Results often appear gradually and build over time. Success is tied to injury severity and tissue quality. Age, health, and activity level also play roles.
Surgery often has clearer structural endpoints than injections. A repaired tendon can be confirmed during the operation. A replacement joint can correct severe arthritis pain. Many procedures have well-studied outcome data across many years.
Still, outcomes vary by surgeon and rehabilitation quality. Stem Cell Therapy vs Surgery often becomes a choice between biologic support and structural reconstruction.
Some patients prefer to try conservative care first. Others need a faster mechanical fix for function. Long-term success also includes lifestyle and weight management. Strength and mobility training help both paths.
Smoking and poor sleep can slow healing for any option. A realistic plan includes both medical care and daily habits.
Questions to Ask Your Doctor Before Choosing a Treatment
Start by asking what is actually causing your symptoms. Ask if imaging matches your pain location and pattern. Clarify whether the condition is mild, moderate, or severe. Ask what treatments are reasonable at your stage.
Discuss what happens if you do nothing for now. These questions help you avoid unnecessary procedures.
Ask about expected timelines for recovery and activity return. Ask what rehab will look like after each option. Ask about risks based on your health history. Bring up medications, blood thinners, and past reactions to anesthesia.
Your doctor should explain the benefits, limits, and uncertainties in plain language. If answers feel rushed, seek a second opinion.
Also ask about cost, coverage, and follow-up care plans. Some regenerative treatments are not fully insured. Ask what happens if the first treatment fails.
Ask whether surgery remains an option later. Ask what success looks like in measurable terms.
How Lifestyle Goals Influence Your Treatment Choice
Your lifestyle goals should shape the treatment plan. Some people need a quick return to work duties. Others care most about long-term comfort and endurance.
Athletes may value joint preservation and flexibility. Parents may need minimal downtime for caregiving tasks. Travel plans and job demands can also affect timing.
Stem Cell Therapy vs Surgery can feel different in daily life. Stem cell therapy may allow faster basic activity return. Surgery may require strict restrictions and structured rehab visits.
Some people can commit to long rehab with strong support. Others need simpler recovery with fewer barriers. The right choice supports your goals, schedule, and tolerance for recovery demands.
Talk with your doctor about what activities matter most to you. Discuss lifting, kneeling, running, or long-standing requirements. Share your pain triggers and your best days too.
A plan should address strength, movement, and inflammation control. Nutrition and sleep also support recovery across both paths. When your goals are clear, the decision becomes easier.